This week, I want to cover a long-standing DME behemoth - Apria Healthcare. Apria which happens supplies DME to roughly 1.8 million people annually across 275 branches. This piece will be a bit shorter than last week - no “smoking guns” like Adapt’s recent executive turnover and organic growth doubts - but still worth covering to understand the market.
Some key differences here - for one, Apria has been around since 1995 - the product of a $1B merger between two dominant California suppliers. Since then, Apria Healthcare has went through a number of owners and has gone public twice - once in 1995, going private in 2008, and then IPOing again this year. Another difference here is key executive tenure - Apria’s current CEO Daniel Starck had significantly more operating experience in the DME industry than Adapt’s first CEO Luke McGee, who resigned just last year. Adapt’s current CEO has comparable experience but has been onboard for a very short time, and initially as a co-CEO (prior to McGee’s departure). So, have these differences in DNA affected how these businesses are run, or are they mostly cosmetic in nature? Let’s dive in and find out.
A Snapshot
Apria Healthcare is one of the top 2-3 domestic DME players today. In 2020, the company earned more than $1B in net revenue and made ~2.4 million deliveries. Interestingly, ~80% of this revenue comes from its oxygen-related products for Obstructive Sleep Apnea (OSA) and home respiratory usage. My gut tells me this focus comes from the ARR driven by supply reorders (diabetes management being the other main DME segment where ARR is generated from the same patient over time). ~20% of their revenue comes from the Kaiser Family Health Plan alone, and overall 80% of their revenue comes out of 1,600 commercial plans (includes Kaiser) that they have contracted with.
According to its 10K, Apria uses just five suppliers to source 75% of its DME. Apria undoubtedly receives major discounts through these supplier contracts through volume, but as we’ve seen throughout the pandemic, failing to diversify your procurement sources can greatly increase your risk of product shortages - I’ll cover this via real-life example in my next piece.
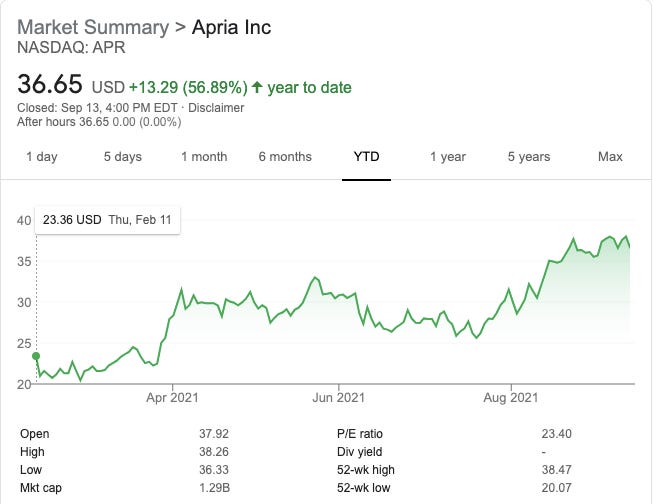
Apria IPO’d in February of this year - probably driven by majority investor Blackstone’s desire for liquidity in their investment. Until recently, it’s been pretty rare for DME companies to go public - but with Adapt, Apria, and shortly RoTech going public recently, we may see more large DME players take a chance with public market financing. Anyways, Apria’s first few quarters as a public company have been phenomenal for public investors thus far (see below). Let’s just say if you bought this stock in February, I am very jealous (still waiting for my IMAX, Planet Fitness, and TripAdvisor COVID buys to turn around…ugh).
Apria’s 25 Year Journey
Apria has seen its fair share of roadblocks to get here though, starting from day 1 integration problems between HomeMedCo and Abbey Healthcare (the CA DME companies). As is the case for most DME M&A, the HomeMedCo/Abbey marriage was consummated to expand their overall reach while leveraging each individual firm’s competitive advantages. Unfortunately, the reality didn’t play out like the expectation - a nontrivial number of the two firm’s branches and employees were deemed redundant by management. As a result, Apria collapsed 525 branches into 350 (275 today) and laid off more than 1,000 employees (~10% of its workforce). To top it off, the firms had been using disparate software - leading to another fun, time-consuming integration challenge.
The post-merger layoffs and technology issues were not the end of Apria’s struggles. Year after year of earnings disappointments led to the exit of Apria’s COO in 1998, and in 2005, Apria put itself up for sale to take itself off the public market. Unfortunately for Apria, investors didn’t bite, and it wasn’t until 3 painful years later that Blackstone came in to take the company private. PE firms obviously aren’t charities - and as you would expect, costs were cut (and labor is a hell of a cost). Blackstone’s ROI expectations, combined with downward Medicare and commercial payor reimbursement trends, led to a 33% decrease in staff over the last decade - from a peak of 9,500 in 2012 to 6,300 as of 2021.
Unexpected integration issues, poor earnings growth, going private to stay alive, dwindling reimbursement. What could be next for Apria? Ah yes, a government lawsuit. Various states AGs, including now DHHS secretary Xavier Becarra, sued Apria for violating the False Claims Act. The states alleged that Apria submitted false claims for Non Invasive Ventilators (NIVs), which were not being used sufficiently by patients - aka Apria’s staff wasn’t actually checking to see if patients were using the equipment. These states also claimed that Apria improperly waived copays to induce beneficiaries to rent NIVs that were more expensive than other, equally effective models. Apria settled, ultimately paying $40 million to the federal government and the states. Beside the reputation stain, Apria had to undertake certain obligations designed to promote compliance with federal healthcare programs, including setting up a corporate compliance office.
Not to fear though, Apria went public shortly after the NIV settlement, and then rewarded its Blackstone investors with a hefty dividend. Apria Healthcare is still kicking - and doing pretty well for themself while they’re at it.
Apria for Patients
With more than 25 years of doing home medical equipment, long-standing relationships with payors and providers, and a seasoned exec leadership team, you’d think Apria would be pretty d*mn good at getting patients what they need, when they need it, right? There must be a reason their number one company tenet is “Patients Rule”, yes?
Ehh…this is American healthcare.
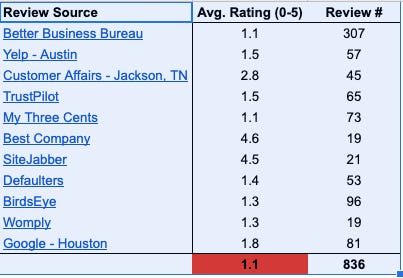
Sure, 800/1,800,000 is ~.05% of people using Apria-supplied DME each year. Further, people who tend to write these reviews are generally the passionately for or against - bias noted. That said, it’s hard not to track the similarity of these complaints to those of AdaptHealth - unresponsive customer service (hours of waiting on hold), excess rental billing after usage, refusal to repair or replace defective equipment, failure to deliver in a timely fashion, etc.
How does one of the largest home healthcare equipment company in the domestic US, a company that has gone through as Apria has over two decades, still SUCK at basic customer service? What can be done differently, if anything?
A Different Route
My main takeaway from researching companies like Adapt and Apria and interviewing stakeholders at Home Health Agencies (HHAs), DME suppliers, and SNFs is that nobody believes there’s margin in doing DME right by the patient. I get it - the stakeholder incentives and dwindling reimbursement rates have made this a very hard business to operate in at all, let alone well. And I’m not here to just “dunk” on the big, easy targets. At least Apria picks up the phone when you call (even if you’re on hold for awhile), which is more than what some of the less savory, smaller DME suppliers can say.
Is there another growth strategy that works within our regulatory and incentive frameworks? Perhaps the best you can really do to service this market is to acquire everything you see and centralize the RCM, procurement, and customer service functions, as companies like Adapt and Apria have. Still, I get nervous when the PE guys are calling the shots (blame my New Yorker subscription!!!). Millions of people depend on this equipment for their quality of life / survival / treatment - not quite sure your family member’s access to oxygen tank supply should hinge on the quarter-to-quarter reactions of PE and the Street.
In the long term, I think the solution is better government policy at the state and federal level - in a way that’s better tethered to the on-the-ground experiences of providers and their patients. As clever as a business plan/model is, there’s only so much change you can effect in US Healthcare without being an elected politician. That’s just my two cents, and I know there are good reasons to disagree, but this is my piece - so you’re getting my opinion.
In the interim, I believe there may still be novel solution to build a sustainable, people-centric DME service. I’m still exploring these potential paths myself - like providing adjacent value-add services to other parts of healthcare ecosystem. You’re seeing a few start ups in the last five or so years try out models too - Parachute Health (health systems) and Tomorrow Health (payors) are two that come to mind - which is most certainly a net good. I’m in the process of developing a Texas-based twist, one with an emphasis on local, quality suppliers. Maybe that’ll end up not being tenable, but hey, I’m a sucker for small business.
Hope you enjoyed this week’s piece! Next time, I’ll cover the massive Philips respiratory recall from earlier this year. In the meantime, feel free to reach out to me to talk Durable, and definitely reach out if you feel that I’ve made a mistake/oversight in my writing.
Have a technical background? Want to solve (or fail to solve, IDK) a cumbersome, opaque industry with regulatory constraints that Kafka wouldn’t wish on his worst enemy?
Former nurse, case manager, people or physical/occupational therapist? Seen these issues occur IRL? Want to get people the DME need easier, and at scale?
In either case, shoot me a message at ed.manzi55@gmail.com. Let’s talk!